Cancer care in Europe: Where are we in 2020?
15.01.20
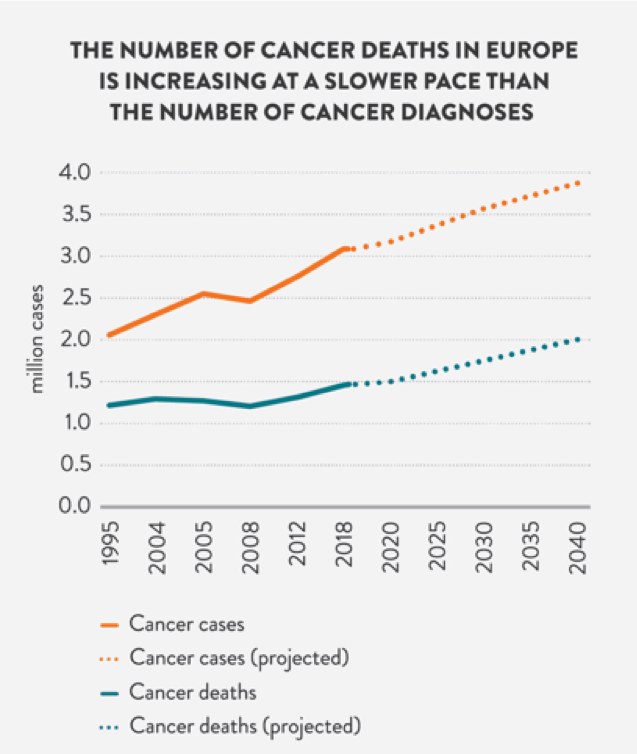
Among the key findings of the Comparator Report on Cancer in Europe 2020, is what looks like a paradox: although more people are being diagnosed with cancer, a smaller proportion of those people appear to be dying from the disease. The report, a comprehensive overview of major cancer trends across Europe, quickly unravels the mystery.